
Tongue Health
Glossitis: Types, Symptoms, Causes, & Treatment
Glossitis is the medical term for an inflamed tongue. When you suffer from glossitis, your tongue may swell, change in color, and alter its texture, potentially affecting your ability to eat or speak comfortably. This condition can arise from various factors, including allergies, physical trauma, and nutritional deficiencies, with treatment approaches varying based on the underlying cause. This article will delve into the causes and different types of glossitis, outline common symptoms, and discuss the treatment methods employed.
Key Takeaways
TABLE OF CONTENTS

TABLE OF CONTENTS
What is Glossitis?
Before discussing symptoms and treatment, it’s important to define what glossitis is. Glossitis is an inflammatory condition of the tongue, characterized by swelling and tenderness, along with changes in surface texture and color. In some cases, the papillae—small surface structures that normally give the tongue its textured appearance—may become reduced or lost, causing the tongue to appear smooth or glossy. Glossitis may present acutely, with sudden onset, or chronically, with symptoms that recur or persist over time.
Types of Glossitis
Several distinct types of glossitis exist, and understanding their characteristic symptoms and appearances can simplify diagnosis. These types include:
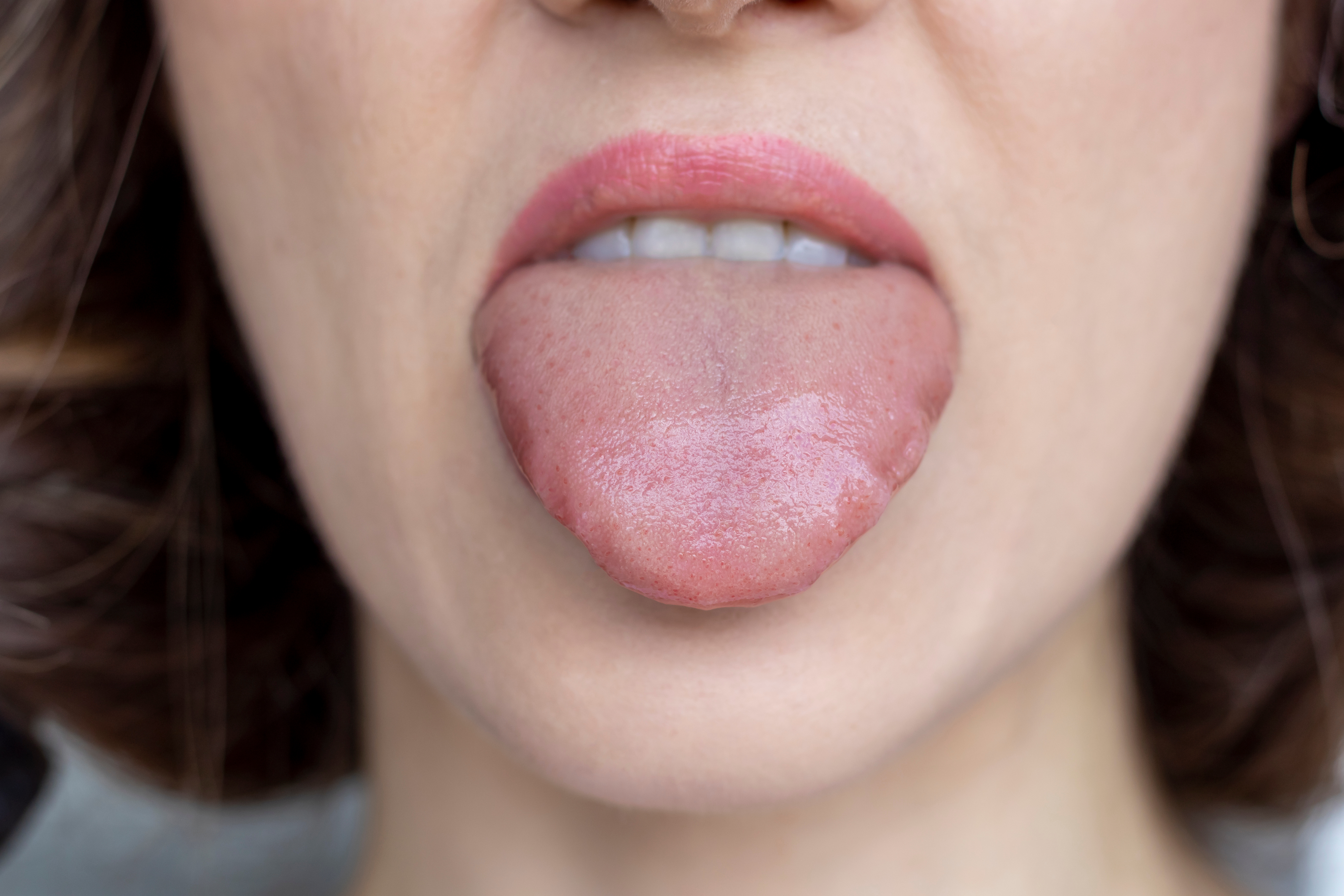
- Atrophic Glossitis: Atrophic glossitis involves atrophy and loss of the papillae on the tongue, altering its normal surface texture. As a result, the tongue may appear smooth, shiny, and sometimes reddened. When atrophic glossitis is associated with vitamin B12 deficiency—most commonly due to pernicious anemia—it is classically referred to as Hunter’s glossitis.
- Median Rhomboid Glossitis: Median rhomboid glossitis typically affects the central, rear portion of the tongue. This area of the tongue becomes red and may either become elevated or swell. Medical professionals generally believe that median rhomboid glossitis signals a fungal infection, specifically oral candidiasis (thrush).
- Burning Mouth Syndrome —also known as burning tongue syndrome—is a chronic pain condition characterized by a burning or scalding sensation in the mouth. The discomfort most commonly affects the tip of the tongue but may also involve the lips, gums, roof of the mouth, or other areas of the oral cavity. Burning mouth syndrome is most frequently observed in peri and postmenopausal individuals, although it can occur in adults of any age.
- Geographic Tongue: Geographic tongue is a benign condition characterized by the sporadic appearance of red, smooth patches across the tongue. These smooth areas often resemble the outlines of countries on a map, which is the origin of the term geographic tongue.

Causes of Glossitis
Glossitis can stem from various sources, and pinpointing the underlying reason is crucial for effective treatment. Common causes of glossitis include:
- Allergens: Frequently, glossitis is triggered by a straightforward allergic reaction. When an allergen or irritant comes into contact with the tongue, it can provoke the papillae to react by swelling or shrinking. Common irritants might include oral care products such as toothpaste and certain medications.
- Disease: Immunodeficiency diseases are known to target the tongue and, in turn, become a cause of glossitis. Herpes simplex (oral herpes), primarily recognized for causing cold sores, can also lead to tongue swelling and irritation.
- Oral Trauma: Injuries to the mouth, including those from accidents, dental procedures, and minor incidents like biting your tongue, can all compromise tongue health and contribute to glossitis.
- Deficiencies: Certain nutrient deficiencies—most commonly iron deficiency (anemia) and vitamin B12 deficiency—can contribute to the development of glossitis. These deficiencies may affect the health of the tongue’s surface, leading to inflammation, tenderness, and a smooth or shiny appearance. In particular, iron and vitamin B12 play important roles in maintaining healthy oral tissues.
- Hormonal Changes: Periods marked by significant hormonal shifts can act as a trigger for glossitis. Burning mouth syndrome is more commonly observed during menopause, though its exact cause remains unclear and is considered multifactorial. For this reason, burning mouth syndrome is sometimes linked to menopause.
- Alcohol and Tobacco Use: Excessive consumption of alcohol or tobacco can negatively impact the health of your tongue and its papillae, leading to glossitis.
Is Glossitis Contagious?
Whether glossitis is contagious depends entirely on the condition's underlying cause. Glossitis itself is not transmissible, but the root cause of the inflammation can be. For example, if glossitis is induced by an infection like the herpes simplex virus, then the virus can be spread through close contact. When caused by hormonal fluctuations, deficiencies, trauma, or other non-communicable factors, glossitis itself will not be contagious.
Glossitis Symptoms
Glossitis symptoms will vary based on the underlying cause of the condition, yet several symptoms are common across different etiologies, including:
- A smooth and glossy tongue appearance
- Soreness or tenderness in the tongue
- Swelling of the tongue
- Visible redness across the tongue or in specific patches
- An alteration in taste perception
- Difficulty eating or swallowing
How is Glossitis Diagnosed?
If you have observed any of the signs or symptoms of glossitis, you might decide to visit a doctor. To diagnose glossitis, your doctor will examine your mouth and tongue, looking for indicators such as inflammation, redness, tenderness, and missing papillae. Once your doctor has determined if you have glossitis, they may opt to perform additional tests to check for an underlying condition. Blood tests, for instance, might be conducted to screen for viral infections or nutritional deficiencies that could be contributing to glossitis.

Treatment and Recovery
Much like the symptoms, glossitis treatment will depend on the condition's underlying cause. Doctors may recommend several therapeutic approaches, with the most common being:
- Medications: In situations where an infection is the cause of your glossitis, your doctor might prescribe medications such as antibiotics or antifungals for treatment. Since median rhomboid glossitis is typically caused by a fungal infection, doctors frequently prescribe medication as a median rhomboid glossitis treatment.
- Oral Care: Diseases that lead to glossitis can result from bacterial accumulation within the mouth, underscoring the critical importance of proper oral care. Brushing your teeth and tongue twice daily should help minimize bacterial buildup and reduce the risk of developing glossitis.
- Dietary Changes: If nutritional deficiencies are identified as the cause of your glossitis, your doctor may suggest supplements or dietary modifications to restore balanced levels of vital nutrients.
- Learning and Avoiding Triggers: For chronic glossitis cases, it is crucial to identify and avoid triggers or allergens that may provoke its recurrence.
Oral Health Essentials: Your Guide to a Healthy Smile
Your tongue contributes to many everyday actions, from chewing and tasting food to forming words and articulating speech. However, the tongue’s textured surface can trap bacteria and food particles. Over time, this can lead to bad breath, gum issues, and may even affect the health of your teeth. To support a healthy tongue, round out your oral care routine with dedicated tongue cleaning:
- Protect Your Smile with a Crest Pro-Health Toothpaste: Make sure to brush twice a day with a stannous fluoride toothpaste like Crest Pro-Health Advanced Deep Clean Toothpaste. Not only does it help fight cavities and tooth decay, a Crest toothpaste formulated with stannous fluoride also strengthens enamel, fights sensitivity, and provides lasting protection against plaque buildup with twice-daily brushing.
- Rinse with a Crest Pro-Health Complete Clean Mouthwash: Finish your routine with an anti-gingivitis/antiplaque mouthwash to kill bad breath germs, support gum health, and wash away remaining food particles from your tongue and other areas of the mouth.
- Brush 2X/day with an Oral-B iO Electric Toothbrush: An electric toothbrush can remove more plaque bacteria than a typical manual toothbrush, helping you maintain a cleaner, healthier mouth. Many Oral-B iO models even feature a tongue-cleaning mode designed to help you efficiently clear food particles and odor-causing bacteria from the tongue’s surface.
- Pair It with an Oral-B iO Gum & Sensitive Replacement Brush Head: A soft-bristled brush head is ideal for gently but effectively removing bacteria and buildup on the tongue. Apply light pressure and brush from the back of the tongue toward the front to help sweep away debris.
- Stay Hydrated: Drinking water throughout the day supports healthy saliva flow. Saliva naturally helps cleanse the mouth and limits bacterial growth on teeth, gums, and the tongue.
- Maintain a Well-Balanced Diet: Foods high in sugars and acids can promote bacterial growth and contribute to tongue coating and other oral issues. A diet rich in water, fruits, vegetables, and whole grains can encourage a healthier oral environment. When you think about your oral health, don’t forget your tongue. Taking a few moments each day to clean your tongue can help combat bad breath, reduce plaque buildup, and support your overall oral and general health.
TABLE OF CONTENTS

TABLE OF CONTENTS
FAQs

Can glossitis go away on its own?
The course of glossitis depends on its underlying cause. Mild cases related to irritation may resolve on their own with good oral hygiene and by avoiding triggers such as spicy or irritating foods. However, if symptoms persist, worsen, or recur over time, it’s important to seek evaluation from a dentist or doctor. A healthcare professional can help determine the cause and recommend appropriate treatment.

How can I prevent glossitis?
Preventing glossitis begins with maintaining good oral hygiene and adopting an optimal oral care regimen, which includes regular visits to the dentist or dental hygienist. Additionally, avoiding irritating foods, staying well-hydrated, and ensuring adequate intake of iron and B vitamins to support tongue health will help prevent the onset of glossitis.

Does glossitis affect taste?
Yes, glossitis can alter or diminish your sense of taste, particularly if the tongue becomes swollen, smooth, or painful. While it might be tempting to consume richly flavored foods (such as spicy and acidic items), doing so can cause greater discomfort and intensify any burning sensation. The pain level varies depending on the cause, but consuming soft foods is generally recommended.

Is glossitis contagious?
Glossitis itself is not contagious, but if an underlying infection causes it, that condition may be transmissible. It's crucial to receive an accurate diagnosis of how you contracted glossitis and to be prescribed the correct treatment.
Sources
- https://my.clevelandclinic.org/health/diseases/23987-glossitis
- https://www.healthline.com/health/glossitis
- https://www.medicalnewstoday.com/articles/322135
- https://my.clevelandclinic.org/health/diseases/21177-geographic-tongue
- https://my.clevelandclinic.org/health/diseases/14463-burning-mouth-syndrome
- Adam, R. (2020). Introducing the Oral-B iO electric toothbrush: next generation oscillating-rotating technology. International Dental Journal, 70 Suppl 1(Suppl 1), S1–S6. https://doi.org/10.1111/idj.12570
- Cheng, R., et al. (2014). Breath and plaque prevention with cetylpyridinium chloride rinses: clinical meta-analysis. Journal of Dental Research, 93, 573.
- Grender, J., et al. (2022). A 12-Week Randomized Controlled Trial Comparing a Novel Electric Toothbrush With an Extra Gentle Brush Head to a Manual Toothbrush for Plaque and Gingivitis Reduction. Compendium of Continuing Education in Dentistry (Jamesburg, N.J. : 1995), 43(3), f20–f29.
- He, T., et al. (2017). The Case for Stabilized Stannous Fluoride Dentifrice: An Advanced Formulation Designed for Patient Preference. Journal of Clinical Dentistry, 28(4 Spec No B), B1-5.
