
Oral Hygiene
Dental Bone Graft: Process, Purpose & Healing Stages
The bone in our jaw can become compromised and diminish due to gum disease, dental trauma, and tooth extraction. Dental bone grafts are a procedure that replaces lost or missing bone in the jaw, restoring the health of the affected area. Bone grafts are frequently performed before dental implant surgery but can also serve as an independent procedure when the jawbone requires structural support. This article will explore the conditions that may necessitate a dental bone graft, detail how the procedure is commonly performed, and outline a typical recovery timeline.
Key Takeaways
TABLE OF CONTENTS

TABLE OF CONTENTS
What is a Dental Bone Graft?
Before delving into the dental conditions that may necessitate a bone graft, we first need to address the question: "what is a dental bone graft?" A dental bone graft is a common oral surgical procedure designed to support a weakened or diminished jawbone. While variations exist, each procedure involves attaching a bone material to the jawbone to strengthen it. Bone grafts establish a framework upon which your body’s own bone tissue can grow and regenerate, thereby reinforcing and strengthening your jaw. In most cases, one of the following four materials will be used for your dental bone graft:
- Xenografts: Bone sourced from animals, typically cows or pigs.
- Alloplasts: Bone-like material synthesized from artificial substances, including calcium phosphate and calcium sodium phosphosilicate.
- Autografts: Bone harvested from your own body.
- Allografts: Bone obtained from another human, usually a screened cadaver donor. While autografts (using your own bone) are often considered the "gold standard" due to their compatibility, other materials like allografts, xenografts, and alloplasts are highly successful and frequently utilized to avoid creating a second surgical site on the patient.

What Conditions Require a Dental Bone Graft?
Dental bone grafts can effectively treat several oral conditions, including:
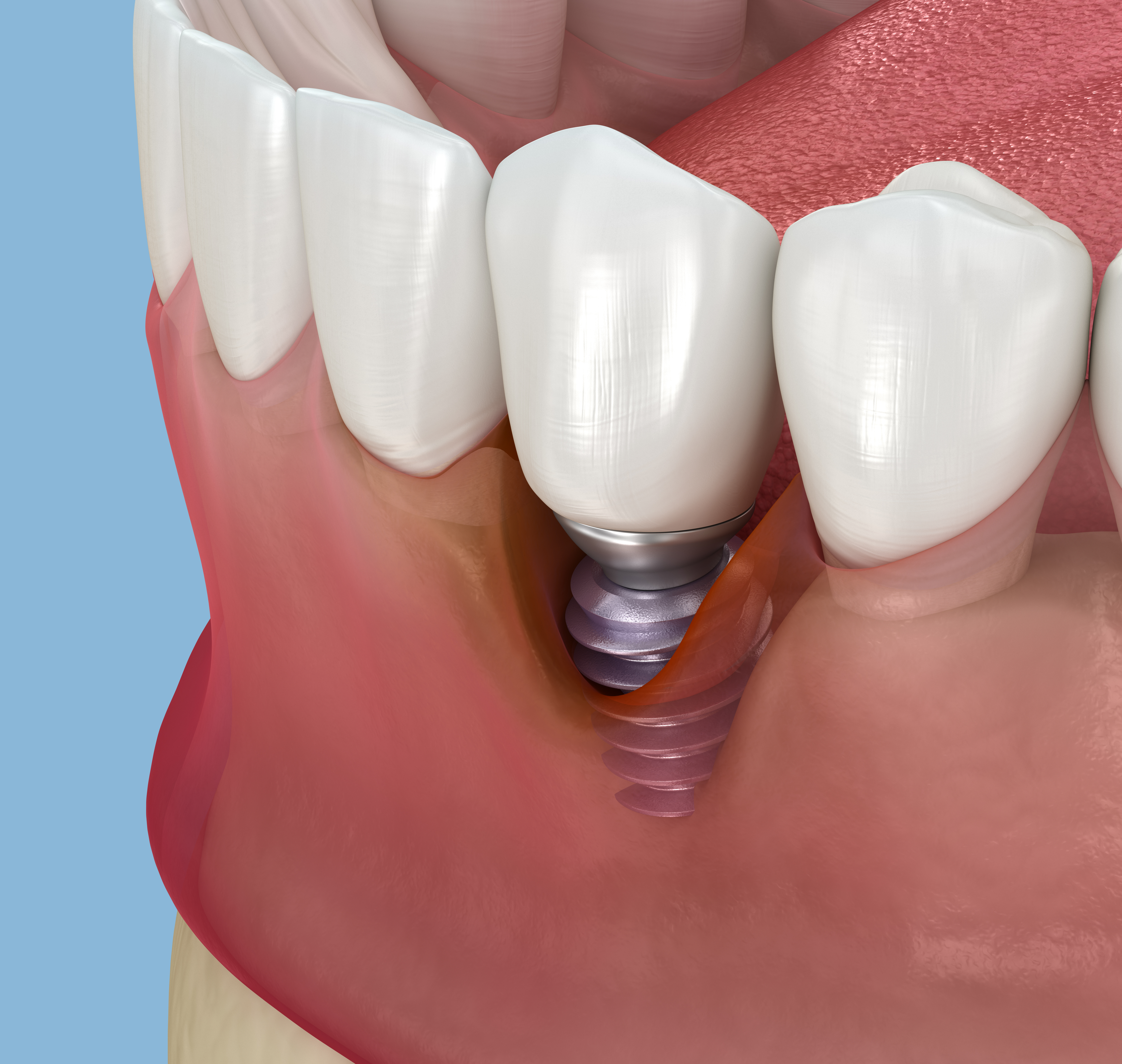
- Tooth Implants Dental implants are used to replace missing teeth by providing a strong, stable foundation for a dental crown. An implant is placed into the jawbone, where it integrates with the bone and functions like an artificial tooth root. In some cases, bone grafting may be recommended before implant placement. This is because a certain amount of healthy jawbone is needed to properly support and hold the implant. Bone grafting helps rebuild or strengthen the bone so the implant can fit securely and function effectively over time.
- Gum Disease In cases of moderate to advanced gum disease (periodontitis), bacteria can damage the jawbone that supports the teeth. When this happens, a dental bone graft may be recommended as part of treatment. Along with periodontal procedures—such as deep cleaning or gum surgery—a bone graft can help rebuild areas of bone that have been lost. Restoring this support can help stabilize the teeth and reduce the risk of further complications from advanced gum disease.
- Loose or unstable teeth that need additional support
- Improving the fit and stability of dentures
- Increasing the width or volume of the jawbone for functional or cosmetic reasons

Dental Bone Graft Procedure
The exact dental bone graft procedure can vary based on where it’s needed in the mouth, but many grafts follow a similar overall approach. Dentists commonly use a few different types of bone grafts, depending on the goal of treatment:
- Block Bone Graft: A small piece of bone is taken from another area of the mouth and used to rebuild bone where significant loss has occurred, often in the front of the jaw.
- Sinus Lift: This type of graft is used in the upper jaw near the back teeth. Bone material is added to increase bone height and create enough support for future dental work.
- Socket Graft: Performed at the time of a tooth extraction, a socket graft helps preserve the bone in the area and reduces the amount of bone loss that can occur after a tooth is removed.
Is a Dental Bone Graft Painful?
A dental bone graft is often a straightforward procedure, and it is performed while the area is fully numbed to keep you comfortable. Even when bone from your own body is used, the process is carefully managed and kept localized, so you should not feel pain during the procedure.
Afterward, it’s normal to experience some mild soreness or a dull throbbing sensation as the area heals. For most people, this discomfort is temporary and can be managed with over‑the‑counter pain relievers. If the procedure is more extensive, your dentist may prescribe medication to help keep you comfortable. Any lingering discomfort typically improves within one to two weeks.
Recovering from a Bone Graft
Recovery from a dental bone graft varies depending on the size of the graft and the reason it was placed. While the full healing process can take several months, the most noticeable discomfort usually occurs during the first week.
In the days following the procedure, it’s normal to experience some swelling, mild bleeding, and soreness around the treated area as the gums begin to heal. Your dentist may recommend or prescribe medication to help manage discomfort and reduce the risk of infection. For most people, pain and swelling improve significantly within about a week.
Over the next several months, healing continues beneath the surface as the jawbone gradually rebuilds and strengthens. During this time, the bone graft supports your body’s natural ability to form new bone. Healing generally progresses through the following stages:
- Early Healing: The gums heal and blood vessels form around the graft to support recovery.
- New Bone Formation: The body begins to grow new bone using the graft material as a framework.
- Bone Strengthening: The new bone hardens and integrates with the jaw, helping restore stability and prepare the area for normal function or future dental treatment.

What Can Influence Healing Time for a Dental Bone Graft?
The size of the graft is not the sole determinant of healing time for a dental bone graft. The following factors can also affect recovery:
- Graft Material: The material chosen for your dental bone graft will influence how long it takes to heal, with each variant integrating at a different rate.
- Underlying Health Conditions: Certain health conditions, including diabetes and autoimmune disorders, can impact the rate at which a bone graft integrates and heals.
- Oral Hygiene: Meticulously maintaining good oral hygiene and adhering to your dentist’s advice following oral surgery minimizes the risk of infection and provides the body with the optimal environment for healing.
- Nutrition: Post-dental bone graft, your dentist may recommend a soft diet or advise against certain foods. This allows the surgical site to heal without disruption from irritants.
- Surgery: The size and complexity of your oral surgery—as well as the techniques used—can influence how long a dental bone graft takes to heal. While it’s natural to want the process to move faster, bone healing follows a natural biological timeline that can’t be rushed.
Maximize Your Dental Health
Good oral care is always crucial, but especially after an oral surgical procedure. Following a dental bone graft, a meticulous and consistent oral care routine is essential to protect the healing site and prevent complications. Immediately after surgery, you should adhere strictly to your doctor’s instructions for your oral care routine.
Oral Health Essentials: Your Guide to a Healthy Smile
Common oral health issues can include cavities, gum disease, staining and sensitivity. The main culprit of which is often plaque buildup—a sticky film of bacteria that forms on teeth. If not treated, cavities and gum disease can lead to tooth loss and may even affect your overall health.
By following a complete oral care routine, you can help nip these issues in the bud, for a stronger, healthier smile:
- Protect your mouth with Crest: Make sure to brush twice a day with a stannous fluoride toothpaste like Crest Pro-Health Advanced Deep Clean Toothpaste. Crest toothpaste formulated with stannous fluoride fights cavities and tooth decay, strengthens enamel, fights sensitivity, and provides lasting protection against plaque buildup with twice-daily brushing.
- Rinse with Crest Pro-Health Complete Clean Mouthwash: Swish with this alcohol-free, antibacterial mouthwash to help rinse away leftover plaque, support gum health, and leave your mouth feeling clean and fresh.
- Brush 2X/day with an Oral-B iO Electric Toothbrush: An Oral-B iO electric toothbrush, helps remove 100% more plaque than a regular manual toothbrush. The dentist-inspired round brush head surrounds each tooth as it adapts to the curves of teeth and gums to ensure a cleaner, healthier smile—even in hard-to-reach areas.
- Use String Floss: Flossing once a day removes plaque and trapped food between teeth. Adding flossing to your routine can help flush away remaining particles and plaque from hard‑to-reach areas, giving you an extra layer of protection and promoting healthier gums.
TABLE OF CONTENTS

TABLE OF CONTENTS
FAQs

How long does it take to heal from a bone graft?
Initial healing after a dental bone graft usually takes a few weeks, but the full healing process—when the graft integrates with your natural bone—often takes three to six months, and sometimes longer depending on the size of the graft and your individual healing response.
During this time, it’s important to keep the area clean, avoid disturbing the graft site, and follow your dentist’s aftercare instructions. Using gentle oral care products and a soft‑bristled toothbrush can help support healing and protect the area as it recovers.
During this time, it’s important to keep the area clean, avoid disturbing the graft site, and follow your dentist’s aftercare instructions. Using gentle oral care products and a soft‑bristled toothbrush can help support healing and protect the area as it recovers.

Is a dental bone graft painful?
During the procedure, your dentist will use local anesthesia, sedation, or general anesthesia to keep you comfortable, so you should not feel pain during the surgery itself.
Afterward, it’s normal to experience some soreness, swelling, or tenderness as the area heals. This discomfort is typically mild to moderate and can usually be managed with over‑the‑counter or prescribed pain relievers. Most people find that discomfort improves significantly within the first week.
Afterward, it’s normal to experience some soreness, swelling, or tenderness as the area heals. This discomfort is typically mild to moderate and can usually be managed with over‑the‑counter or prescribed pain relievers. Most people find that discomfort improves significantly within the first week.

Can I eat normally after a dental bone graft?
After a dental bone graft, your mouth will be sensitive while it heals. For the first few days, it’s best to stick to soft foods to avoid irritating the surgical area.
You should avoid hard, crunchy, spicy, or very hot foods that could disturb the graft site or delay healing. Your dentist will let you know when it’s safe to gradually return to your normal diet.
You should avoid hard, crunchy, spicy, or very hot foods that could disturb the graft site or delay healing. Your dentist will let you know when it’s safe to gradually return to your normal diet.
Sources
- https://www.healthline.com/health/dental-bone-graft
- https://my.clevelandclinic.org/health/diseases/21482-gum-periodontal-disease
- https://my.clevelandclinic.org/health/treatments/21727-dental-bone-graft
- https://www.biosny.com/dental-bone-graft-healing-timeline/
- https://www.mayoclinic.org/tests-procedures/dental-implant-surgery/about/pac-20384622
- Biesbrock, A., et al. (2006). Assessment of treatment responses to dental flossing in twins. Journal of periodontology, 77(8), 1386–1391. https://doi.org/10.1902/jop.2006.050399
- Grender, J., et al. (2022). A 12-Week Randomized Controlled Trial Comparing a Novel Electric Toothbrush With an Extra Gentle Brush Head to a Manual Toothbrush for Plaque and Gingivitis Reduction. Compendium of Continuing Education in Dentistry, 43(3), f20–f29.
- He, T., et al. (2017). The Case for Stabilized Stannous Fluoride Dentifrice: An Advanced Formulation Designed for Patient Preference. Journal of Clinical Dentistry, 28(4 Spec No B), B1-5.
- White D. J. (2005). An alcohol-free therapeutic mouthrinse with cetylpyridinium chloride (CPC)--the latest advance in preventive care: Crest Pro-Health Rinse. American Journal of Dentistry, 18 Spec No, 3A–8A.
